When blood flow to the extremities slows, particularly to the feet, it most likely is caused by a blockage of the arteries. This condition, called peripheral arterial disease (PAD), is very common. Smoking, obesity, poor eating habits, and being sedentary are major factors in the development of PAD. Other maladies, such as diabetes and hypertension, can further cause the blood vessels to narrow. Symptoms of PAD include pain and cramping in the legs and feet when walking, numbness, sores that don’t heal, and foot pain when at rest. Some life changes can help reduce the symptoms, such as lowering fats and cholesterol in your diet, moving around more, reducing stress, stopping smoking, and lowering your blood pressure. If you develop sores on your feet and ankles that refuse to heal, and are experiencing other PAD symptoms, it is a good idea to make an appointment with a podiatrist for an examination and ongoing treatment plan.
Peripheral artery disease can pose a serious risk to your health. It can increase the risk of stroke and heart attack. If you have symptoms of peripheral artery disease, consult with Dr. Castillo from Bronx Foot Care. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
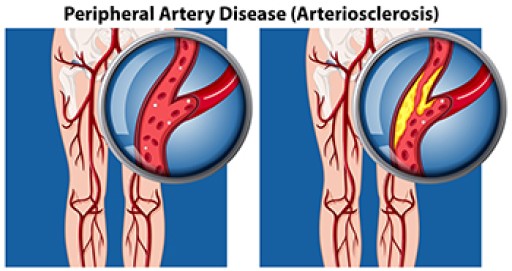
Peripheral artery disease (PAD) is when arteries are constricted due to plaque (fatty deposits) build-up. This results in less blood flow to the legs and other extremities. The main cause of PAD is atherosclerosis, in which plaque builds up in the arteries.
Symptoms
Symptoms of PAD include:
- Claudication (leg pain from walking)
- Numbness in legs
- Decrease in growth of leg hair and toenails
- Paleness of the skin
- Erectile dysfunction
- Sores and wounds on legs and feet that won’t heal
- Coldness in one leg
It is important to note that a majority of individuals never show any symptoms of PAD.
Diagnosis
While PAD occurs in the legs and arteries, Podiatrists can diagnose PAD. Podiatrists utilize a test called an ankle-brachial index (ABI). An ABI test compares blood pressure in your arm to you ankle to see if any abnormality occurs. Ultrasound and imaging devices may also be used.
Treatment
Fortunately, lifestyle changes such as maintaining a healthy diet, exercising, managing cholesterol and blood sugar levels, and quitting smoking, can all treat PAD. Medications that prevent clots from occurring can be prescribed. Finally, in some cases, surgery may be recommended.
If you have any questions, please feel free to contact our offices located in Bronx, NY Yonkers, NY . We offer the newest diagnostic and treatment technologies for all your foot care needs.